An evaluation of the use of reusable theatre hats
By Simon Billingsley
Fourth year medical student at University of Sheffield
|
This essay was one of the runners-up in the 2022 BOA Medical Student Essay Prize How can we make Trauma & Orthopaedics in the UK more Eco-friendly? |
Introduction
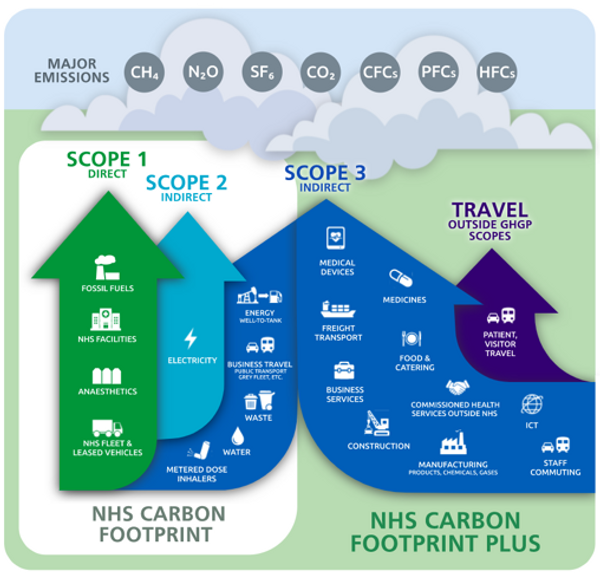
The NHS has a multitude of ways in which it causes environmental harm1 (Figure 1). One area that Trauma and Orthopaedics (T&O) can help is through theatre-wear, more specifically, theatre hats. Disposable viscose hats (DVHs) in NHS surgical theatres are a large contributor to the waste and carbon equivalent footprint that the NHS produces. Switching from DVHs to reusable cloth hats (RCHs) may offer environmental benefits.
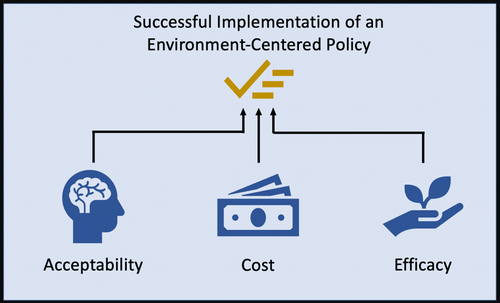
For this change in how T&O operates to be realistic long term, we must consider three main factors (Figure 2) to estimate how beneficial and realistic the change of theatre hat policy would be:
- Acceptability, is it acceptable to all parties involved?
- Cost, is it cost effective?
- Efficacy, does it make T&O more eco-friendly?
Scale
Firstly, the scale of the issue must be appropriately large to warrant a change.
50,272 Orthopaedic Finished Consultant Episodes (FCE’s) that required a procedure took place in the NHS in December 20212. Alongside information on T&O cases per list3 we can estimate the number of theatres lists in T&O per month (Table 1).
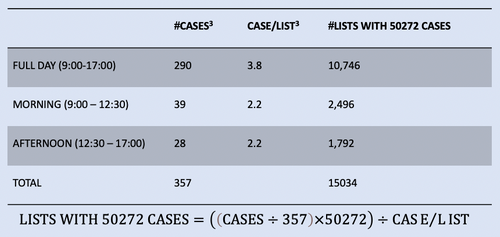
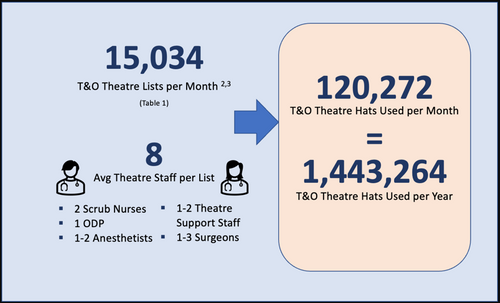
Assuming eight theatre staff per list, the previously calculated 15,034 T&O lists per month2,3 and that each staff member requires one DVH for a list, we arrive at 1,443,264 DVH’s used per year for T&O theatres in the NHS (Figure 3).
Cost
To establish the cost of the proposed policy, we must first know the current expenditure on DVHs.
The average cost of DVHs from 365healthcare is approximately £133.02 per 600 hats4,5 (Figure 4), equating to an annual cost of £319,967.64 for T&O, assuming no waste.

The price of RCHs varies with materials, retailers and number of hats required (Table 2). The rotation of the hats between use, washing and drying requires that more hats are bought than are used in a single day. The optimal number of hats for the rotation will be decided at department level, however, it must be at least double the minimum daily requirement.
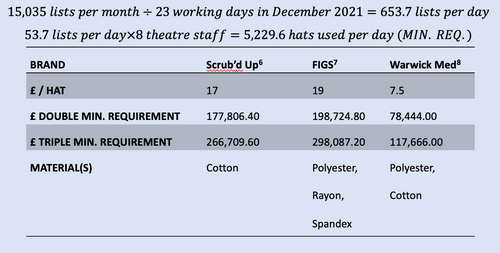
A yearly cost of £319,967.64 is larger than a cost of up to £298,087.20 for RCHs that last approximately three years8.
Post-use cost should also be considered. With the cost per tonne of waste management in the NHS9, we can estimate that T&O spends £947.20 per year managing DVHs after use. This represents another potential cost saving as the yearly laundry cost for the RCHs is estimated to be £594, (Figure 5).
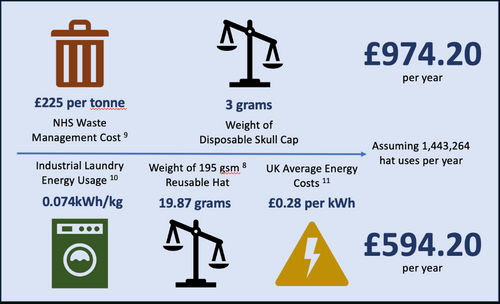
Efficacy
The switch from DVHs to RCHs in T&O theatres has a range of environmental benefits.
The production of RCHs has a reduced environmental impact profile when compared to DVH’s. Being a wood derivative, viscose requires deforestation12, which indirectly raises atmospheric CO2 by reducing photosynthesis capacity. Once the wood is turned into pulp, it is washed and bleached. This process uses large volumes of water, leading to water wastage, in addition to a high energy budget. Additional use of bleach gives rise to a risk of soil and water pollution.
The production of cloth has a less harmful chemical profile and due to the different types of material that can be used the environmental impact is variable, however there is the opportunity for production processes to be altered to become more eco-friendly in-line with the values of the NHS. It is notable that whilst 1,443,264 DVHs must be produced per year, only around 10,459 - 15,688 RCHs would have to be produced every three years.
An additional environmental impact comes from delivery of theatre hats. Although difficult to measure, the annual delivery of 1,443,264 DVHs will have a higher carbon footprint compared to the delivery of 10,459 - 15,688 RCHs every three years.
In terms of end disposal there is no readily available information suggesting that there is a difference between RCHs and DVHs. Similarly, the exact incineration emission profiles of the two materials are not readily available, making for difficult comparison. What can be compared is the volume of hats being disposed. If we assume that both disposable and reusable hats are incinerated and sent to landfill at the same rate, a yearly volume of 1,443,264 vs approximately 5,229.6 is a significant reduction. This is a ratio of approximately 1:289, and if you consider weight (19.87g vs 3g) then that’s a weight ratio of approximately 1:44.
Acceptability
For the policy of switching to reusable hats to be successful, it must be acceptable to the staff, patients and organisation.
Firstly, and most importantly, the new hats must be safe for use in theatres and continue to provide a reduction in surgical contamination and associated infections. Studies show that RCHs allow less contaminants into the operating room atmosphere than disposable ones13, potentially reducing surgical site infections (SSIs). It has also been shown that type of theatre hat has no association to risk of SSI in general surgery14.
Another issue of great importance is wearability. Imperial College London showed an average response of 4.9/5.0 by staff when asked if they’d be happy to try the RCHs15. A large talking point regarding reusable theatre hats is the ability to personalise, being able to present the wearers role or even name. It has been shown that 30-50% of people forget their colleagues’ names after surgical briefing16,17, and that teams work better when they know the names and roles of other members18,19. This is reflected in the polling, with staff almost exclusively saying role-labelled caps would aid communication15. Polling also shows patients welcome the idea with 90% reacting positively20.
Conclusion
T&O goes through approximately 1,443,264 disposable hats per year nation-wide, whereas the same scope of practice would only require 10,459 - 15,888 reusable hats that would last at least three years. This has huge impacts for reducing the polluting process of viscose production, as well as a drastic decrease in landfill and incineration associated pollution, deforestation and delivery associated pollution.
The change to reusable hats would also have financial benefits, potential safety benefits and polling suggests it would be welcomed by staff and patients.
References
- NHS. Delivering a net zero NHS. Available from: www.england.nhs.uk/greenernhs/a-net-zero-nhs. [Accessed 01 February 2022].
- NHS. Provisional Monthly Hospital Episodes Statistics for Admited Patient Care and Outpatients, December 2021: Opeen Data – Treatment Specialty. Available from: https://digital.nhs.uk/data-and-information/publications/statistical/provisional-monthly-hospital-episode-statistics-for-admitted-patient-care-outpatient-and-accident-and-emergency-data/april-2021---december-2021. [Accessed 01 February 2022].
- Hickey BA, Chandratreya AP. Use of theatre time in elective orhopaedic surgery: where does the time go? Royal College of Surgeons of England Bulletin. 2011;93(3):7-9.
- 365 Healthcare. Universal Blue Theatre Caps (Tie Backs). Available from: www.365healthcare.com/Operating-Theatre/Headwear/Theatre-Caps/Universal-Blue-Theatre-Caps-Tie-Backs-~p~UN91220. [Accessed 01 February 2022].
- 365 Healthcare. Universal Blue Theatre Caps (Elasticated Backs). Available from: www.365healthcare.com/Operating-Theatre/Headwear/Theatre-Caps/Universal-Blue-Theatre-Caps-Elasticated-Backs-~p~UN91230. [Accessed 01 February 2022].
- Scrub’d Up. Scrub’d Up. Available from: www.scrubdup.com. [Accessed 04 February 2022].
- FIGS. Modern Classic Scrub Cap. Available from: www.wearfigs.com/products/unisex-modern-classic-scrub-cap-scrub-cap?color=Navy. [Accessed 04 February 2022].
- Warwick Med. Warwick Med. Available from: www.warwickmed.co.uk. [Accessed 04 February 2022].
- Rose Gallagher. Freedom of Information Follow up Report on Management of Waste in the NHS. Royal College of Nursing. 2018.
- CINET Professional Textile Care. Industrial Laundry up to 3 times more sustainable compared to household washing and drying. Available from: www.cinet-online.com/uploads/files/CINET_Industrial%20Laundry%20(1).pdf. [Accessed 06 February 2022]
- Erin Yurday, NimbleFins. Average Cost of Electricity per kWh in the UK 2022. Available from: www.nimblefins.co.uk/average-cost-electricity-kwh-uk. [Accessed 06 February 2022].
- TheatreCaps. Greener. 2020. Available from: https://theatrecaps.com/blogs/theatrecaps-blogs/go-green. [Accessed 07 February 2022].
- Markel TA, Gormley T,, Damon Greeley D, et al. Hats Off: A study of Different Operating Room Headgear Assessed be Environmental Quality Indicators. J Am Coll Surg. 2017;225(5):573-81.
- Haskins IN, Prabhu AS, Krpata DM, et al. Is there an association between surgeon hat type and 30-day wound events following ventral hernia repair? Hernia. 2017;21(4):495-503.
- PatientSafe Network. 725E0E4C-29C7-41D9-8598-00C9E2FE2206. 2019. Available from: www.psnetwork.org/725e0e4c-29c7-41d9-8598-00c9e2fe2206. [Accessed 10 February 2022].
- Birnbach DJ, Rosen LF, Fitzpatrick M, et al. Introductions During Time-outs: Do Surgical Team Members Know One Another’s Names? Jt Comm J Qual Patient Saf. 2017;43(6):284-8.
- Burton ZA, Guerreiro F, Turner M et al. Mad as a hatter? Evaluating doctors’ recall of names in theatres and attitudes towards adopting #theatrecapchallenge. Br J Anaesth. 2018;121(4):984-6.
- Bobb MR, Ahmed A, van Heukelom P, et al. Key High-efficiency Practices of Emergency Department Providers: A Mixed-methods Study. Acad Emerg Med. 2018;25(7):795-803
- Leonard M, Graham S, Bonacum D. The human factor: the critical importance of effective teamwork and communication in providing safe care. BMJ Quality & Safety. 2004;13:i85-i90.
- PatientSafe Network. 8A110CE3-08F5-4751-AA59-6367E825B3B5. Available from: www.psnetwork.org/theatrecapchallenge-wheres-the-evidence/8a110ce3-08f5-4751-aa59-6367e825b3b5. [Accessed 12 February 2022].
