Gender equity, waiting lists and the trauma and orthopaedic profession
By Meryam Benaichouche
5th year medical student at University College London
|
This essay was a runner-up in the 2023 BOA Medical Student Essay Prize With the changing demographics and working practices within T&O, how can we sustain the workforce and standards of care currently provided within the NHS? |
Given the UK’s ageing demographic, T&O doctors are forced to confront problems of chronic pain and non-urgent presentations leading to a rise in elective procedures, such as elective joint replacements (EJR), and outpatient referrals1. However, the seismic disruption of COVID to ‘non-essential operations’2 have led waiting times for non-urgent interventions and elective surgical procedures to rise exponentially. This is troubling given that significant delay of EJRs - including ‘the operation of the century’3, the total hip arthroplasty - can lead to deterioration of physical, mental and social wellbeing4. Sustaining and improving standards of orthopaedic care since COVID, and improving patient quality of life, now desperately rely on managing both the patients on the waiting lists, and actively managing the waiting list itself. All of which are impossible tasks without a sustainable workforce. This piece will focus on addressing waiting times as a key intervention for upholding standards of care, and efforts towards gender equity in T&O as a means of sustaining the workforce long-term.
Sustaining standards of care
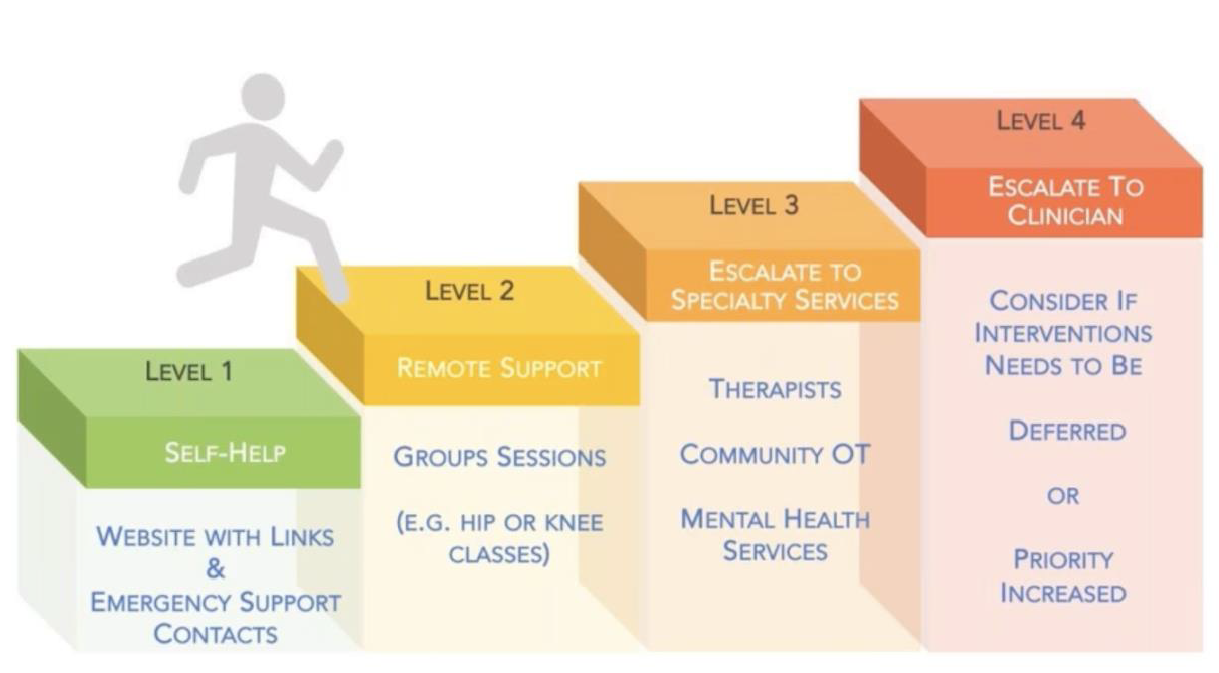
Managing waiting patients requires T&O departments to work with primary care networks to create soft interventions; a supportive, scalable sequence of resources (Figure 1) that allows patients to self-manage during the waiting period to prevent physical and mental health deteriorations5. Managing the waiting list itself involves a review process that assesses present condition and reprioritises patients according to need. The benefits of this dual approach are two-fold. Firstly, preventing further health deterioration. Secondly, optimising patient engagement during normally silent waiting periods. Surveys5 point to a lack of clarity and anxiety, and not just ongoing pain, as reasons for poor patient feedback. Acting on these concerns, notwithstanding the larger, arduous task of cutting waiting times, can massively increase patient satisfaction rates.
A patient-supported blend of digitalisation in the form of video consultations and telephone follow-ups for those who do not need in-person assessment can also serve to cut waiting times. Patient initiated follow up (PIFU) systems, modelled and implemented effectively in a minority of trusts7, have been shown to reduce up to a third of outpatient appointments (Table 1) when patients' conditions are stable.
| Specialty | Appoitments avoided per patient on a PIFU |
| Audiology | 1.77 |
| Trauma and orthopaedics | 1.24 |
| Rheumatology | 1.08 |
| Ear, nose and throat | 0.96 |
| Urology | 0.83 |
| Pain management | 0.81 |
The suggestions above share an increased role of patients in managing their conditions. Such interventions are framed in the literature as 'patient-led' or as promoting patient 'ownership'. Whilst true from one viewpoint, it is important to acknowledge a shift in the duty of healthcare provision and recent trends in redistributing much of this labour to the patient. The ability of patients to take up this labour falls along existing structural, socio-economic and racial inequalities which risk deepening ‘health inequity’8.
Sustaining the workforce: Recruitment, retainment, retirement
A survey9 of the T&O workforce anticipates a capacity gap due to early retirement by senior clinicians, delays in qualification secondary to reduced training opportunities for current trainees and anticipated poor recruitment. Equally important are poor perceptions of the T&O specialty amongst students, particularly female medical students, and the inevitable effects of this on perpetuating future recruitment bottlenecks. Sustaining a workforce thus requires tapping into groups of doctors past, present and - the focus of this piece - future.
Recruitment: A 'feminist' take
The direct progression of doctors into specialty training after the foundation programme has fallen to almost 30%10 with ‘low morale, disconnect, unmanageable change and lack of personal and professional support’ being cited as leading causes11. With over half of training doctors being women12, T&O, a specialty where 92% of consultants are men, is placed in a uniquely precarious position. Gender equity in T&O hereby becomes an urgent matter of sustaining staff quality and quantity. Though legitimate efforts to increase the visibility of women in T&O exist, the reality is that 'women in surgery' events alone do not alter negative perceptions of discrimination and gender bias in orthopaedics13. T&O faculties with greater female faculty members expectedly recruit more female trainees but accepting that 'representation' may not be a reality for all T&O programs at this stage is the first step in sincerely tackling the gender divide in orthopaedics. Prioritising opportunities for female medical students to access T&O surgical mentorship and teaching is definitively more effective at creating and sustaining interest and should trump visibility-centred catchphrase sloganeering. Male mentorship, when positive and sincere, is equally effective14. Involving male members in the institutional effort through formal mentorship schemes not only increases job satisfaction amongst consultants but helps to create a co-led interest in gender equity. One whereby gender equity is a shared task and shared responsibility.
Conclusion
The influence of government imperatives on NHS services necessitates a state-driven model of healthcare delivery that increasingly crafts healthcare users as co-producers of and collaborators in healthcare delivery15. As individuals to be ‘cared for’16, sometimes before illness has even taken place, in the form of preventative strategies and community-based social care measures17. This evolution attempts to serve a complex ageing population with multiple morbidities and social care needs, but has, in the process, redirected limited financial resources away from acute or hospital-based services. The effect of this on the surgical workforce, particularly providers of elective surgeries such as T&O, is increased rates of burnout and low levels of self-esteem and motivation. The task of addressing waiting lists seems sisyphean and introducing clinician-led strategies to manage waiting lists is crucial in moving forward. Furthermore, anticipated bottlenecks in recruitment highlight why gender equity in T&O is everybody’s problem. Well-meaning strategies, which focus on female visibility, replicate labour inequalities by framing gender issues as exclusively ’women’s work’. In T&O, men must be encouraged into positions to positively and actively affect various scales of change, even if it is more appropriate for such efforts to be driven by female leadership. It is increasingly apparent that 92% of T&O leadership cannot simply ally itself but must help steer the ship.
References
- NHS England (2017). Transforming Musculoskeletal and Orthopaedic Elective Care Services a Handbook for Local Health and Care Systems. [online]. Available at: www.england.nhs.uk/wp-content/uploads/2017/11/msk-orthopaedic-elective-care-handbook-v2.pdf.
- Bayley M, Goubran A, Salar O, Toms A, Howell J. The Change in Practice in the Trauma and Orthopaedic Department in the Royal Devon and Exeter Hospital and the Influences for the Post-COVID-19 Era of the National Health Service. Orthopaedics Onine. [British Orthopaedic Association). Available at: www.boa.ac.uk/resources/the-change-in-practice-in-the-trauma-and-orthopaedic-department-in-the-royal-devon-and-exeter-hospital-and-the-influences-for-the-post-covid-19-era-of-the-national-health-service.html [Accessed 20 Feb. 2023].
- Learmouth ID, Young C, Rorabeck C. The Operation of the Century: Total Hip Replacement. Lancet. 2007;370(9597):1508-19.
- Scott CEH., Turnbull GS, Powell-Bowns MFR, MacDonald DJ and Breusch SJ. Activity levels and return to work after revision total hip and knee arthroplasty in patients under 65 years of age. Bone Joint J. 2018;100-B(8):1043-53.
- Kulkarni K, Shah R, Armaou M, Leighton P, Mangwani J and Dias J. What can we learn from the experiences and expectations of patients on growing waiting lists for planned care in the COVID-19 pandemic? Bone Jt Open. 2021;2(8):573-83.
- Dias J. Coping with COVID: Managing recovery and supporting patients [Webinar]. 2020. Available at: www.boa.ac.uk/learning-and-events/webinars/coping-with-covid-webinar-series/coping-with-covid--may-2021-rec.html. (Accessed: 21 February 2023).
- NHS England (2022). Implementing patient initiated follow-up Guidance for local health and care systems. Available at: www.england.nhs.uk/wp-content/uploads/2022/05/B0801-implementing-patient-initiated-follow-up-guidance-1.pdf. [Accessed 22 Feb. 2023].
- Marmot M. Fair Society, Healthy Lives the Marmot Review. [Online]. 2010. Available at: www.parliament.uk/globalassets/documents/fair-society-healthy-lives-full-report.pdf. [Accessed 22 Feb. 2023].
- British Orthopaedic Association. Workforce Surveys. [online] Available at: www.boa.ac.uk/policy-engagement/workforce-surveys.html. [Accessed 19 Feb. 2023].
- UK Foundation Programme Office (2020). F2 Career destination report 2019. Available at; https://foundationprogramme.nhs.uk/resources/reports. [Accessed 19 Feb. 2023].
- Andah E, Essang B, Friend C, Greenley S, Harvey K, Spears M, Reeve J. Understanding the impact of professional motivation on the workforce crisis in medicine. BJGP Open 2021;5(2):BJGPO.2021.0005.
- General Medical Council (2019). The state of medical education and practice in the UK. The Workforce Report 2019. Available at: www.gmc-uk.org/-/media/documents/the-state-of-medical-education-and-practice-in-the-uk---workforce-report_pdf-80449007.pdf. [Accessed 20 Feb. 2023].
- Hull B, Pestrin O, Brennan CM, Hackney R, Scott CEH. Women in Surgery Events Alone do not Change Medical Student Perceptions of Gender Bias and Discrimination in Orthopaedic Surgery. Front Surg. 2022:9:905558.
- Green J, Chye V, Hiemstra L, Felländer-Tsai L, Incoll I, Weber K, et al. Diversity: Women in orthopaedic surgery -a perspective from the International Orthopaedic Diversity Alliance. Journal of Trauma and Orthopaedics. 2020;8(1):44-51. Available at: www.boa.ac.uk/static/a24ead71-ad82-4e23-98efacf343cbd015/Diversity-women-in-orthopaedic-surgery-IODA-perspectiveupdated-110320.pdf. [Accessed 22 Feb. 2023].
- Howieson B. The mutuality metaphor: Understanding healthcare provision in NHS Scotland. J Health Organ Manag. 2016;30(4):666-71
- Kyratsis Y, Atun R, Phillips N, Tracey P, George G. Health systems in transition: Professional identity work in the context of shifting institutional logics. Academy of Management Journal. 2017;60(2):610-41.
- Martin G, Bushfield S, Siebert S, Howieson B. Changing Logics in Healthcare and Their Effects on the Identity Motives and Identity Work of Doctors. Organization Studies. 2021;42(9):1477-99.
