Orthopaedic surgeons as vaccinators: playing our part in the pandemic
By Pranai Buddhdev, Thomas Stringfellow, Albert Ngu, Hilary Bosman, Andy MacDowell, Roland Russell and William Martin
Department of Trauma and Orthopaedics, Broomfield Hospital, Mid and South Essex NHS Foundation Trust
Introduction
The vaccination programme was launched in our trust at the end of December, following the guidance as suggested by Joint Committee on Vaccination & Immunisation (JCVI) with regards to priority groups including those at risk who are over 80, those residing in care home and healthcare workers. There became a need for further volunteers to assist in the vaccination effort, and as a department both consultants and registrars were actively encouraged to aid the service. Reassuringly, Ferguson et al. concluded that trainees can continue to make adequate progress towards orthopaedic trauma indicative numbers whilst assisting in other hospital departments during elective surgery pauses1.
Vaccinator training programme
This involved successful completion of seven online training modules and assessment2 which can be accessed through the NHS Health Education England e-LFH platform including:
- Legal aspects of vaccination
- Vaccine storage
- Vaccine administration
- Recognising and managing anaphylaxis
- Core knowledge for COVID-19 vaccinators
- COVID-19 Pfizer vaccine
- COVID-19 AstraZeneca vaccine
Each of these took around 20-30 minutes to complete, with certification that was forwarded to the vaccine programme co-ordinators. The Green Book on Vaccination Coronavirus chapter (14a) provides answers to many questions that patients and colleagues may have about the vaccines and is a reliable source of information3.
Following this, an in-person assessment was completed, specifically with regards to the safe reconstitution of the Pfizer vaccine into a dispensable form with clear documentation of times as noted by a member of the pharmacy team. Each vial is made by adding 1.8ml 0.9% saline which allows for 6 doses from each vial of 0.3mls each4. In order to account for the number of vaccine doses dispensed, each dose volume is checked by a roaming healthcare professional and the vaccinator is unable to leave the immediate area unattended until the vial has been completely utilised. The vaccine is given by an intramuscular injection into the deltoid muscle and patients are required to stay in a waiting area for 15 minutes after their dose to monitor for anaphylaxis (Fortunately, this hasn’t happened whilst any of us have been vaccinating!).
Currently, the Pfizer vaccine is being dispensed in our hub due to its availability and stringent storage methods, however it has been reported that AstraZeneca has ramped up manufacturing of the AstraZeneca Oxford vaccine with the aim of producing 2 million doses per week5. It is likely that this will be dispensed more in the community and at smaller vaccination hubs in the future due to easier storage and transportation guidelines. We have described the pertinent differences of the two vaccines below and encourage all healthcare professionals to be aware these (Table 1).
|
Vaccine |
Pfizer BioNTech162b24 |
AstraZeneca (Oxford)6 |
|
Type |
mRNA nanoparticle vaccine |
Non-replicating adenovirus vector vaccine |
|
Licence |
>16 years of age |
>18 years of age |
|
Clinical trials |
44,000 Patients (6 countries) |
24,000 Patients (3 countries) |
|
Vaccine efficacy |
up to 95% |
up to 70.4% |
|
Dose |
0.3 ml |
0.5 ml |
|
No. doses per Vial |
5–6 |
8–10 |
|
Storage |
-80°C – -60°C (freezer) → thawed to +2°C – +8°C |
+2°C – +8°C |
|
Shelf-life at Room Temp |
6 hours (once reconstituted) |
6 hours |
|
Manufacturer 2nd dose recommendation |
3–12 weeks post dose 1 |
4–12 weeks post dose 1 |
Table 1. Summary of vaccine properties and product characteristics. Information from medicines and health products regulatory authority summary of product characteristics documents (SPC)4,6.
Legal aspects of vaccine administration
Nursing staff and allied healthcare professionals without prescribing rights may administer the vaccination under a patient group directive (PGD) whereby a dose can be given to any patient covered by the PGD without a patient-specific prescription7. PGD’s currently cover the patient groups mentioned above, doctors are not currently permitted to administer the vaccine under a PGD and must instead prescribe each individual dose given for each individual patient, a patient specific directive (PSD)7. Our experience has been each PSD requires slightly more paperwork (and therefore time) per dose than that administered under a PGD.
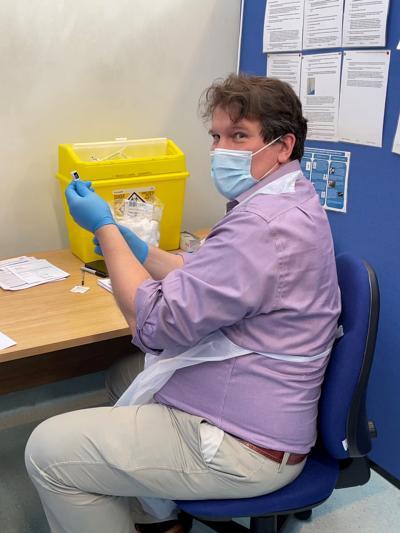
Personal experience: Trauma and orthopaedic registrar
Firstly doctors, secondly orthopaedic surgeons, is certainly our current mantra as we live through ‘the third lockdown’. Registrar colleagues around the UK will be having all kinds of different experiences again, ICU and medical redeployment, proning and emergency department cover whilst running our (albeit, slightly) quieter trauma services. In between shifts taking direct referrals from minor injuries and the emergency department, staffing fracture clinics and maximising time in trauma theatre we have found some time to take part in the vaccination effort.
This has been an entirely voluntary choice by my colleagues and me, choosing to help meet local demand for vaccination on zero days and extra shifts. The training takes around half a day in person at our centre and was a great opportunity to meet other staff in the hospital. Each vial of six doses takes around 30 minutes to administer and there is a great atmosphere among patients and staff alike. Ultimately, whilst this is not going to help with operative numbers or CCT requirements it is extremely rewarding and certainly lifts the spirits knowing each vaccination is one small step closer to normality!


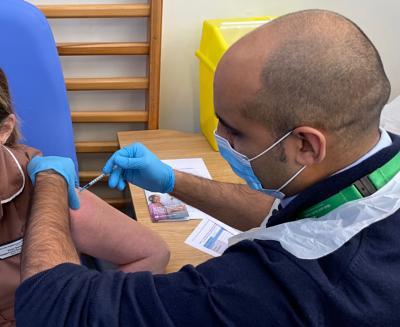
Personal experience: Trauma and orthopaedic consultant
There has been a concerted effort from my colleagues to be part of the vaccinator team, to feel productive and fulfilled during this current lockdown where we have, once again, seen our elective workload decimated. We have continued to perform emergency operations, take direct MSK referrals from ED to the fracture clinic, perform telephone consultations and stratify waiting lists whilst volunteering our ‘elective theatre sessions’ to the vaccination hub efforts.
As surgeons, it has been a truly rewarding experience; preserving patient contact and noting the appreciation from those most vulnerable including some of our own theatre, clinic and administrative staff! There has been a very collegiate atmosphere, working side by side with many members of staff we do not commonly interact with regularly, and this positive working environment has led to some colleagues volunteering their time on weekends to local hospital and community vaccination efforts.
Conclusion
Becoming a vaccinator does require time and motivation to complete the training, however, we are all very re-assured by this process and it is clear from our experience that all vaccinators are knowledgeable and carry out their duties with great care. It is a very fulfilling role and patients are incredibly grateful for our efforts. As different geographical areas and units adapt and respond to fluctuating infection levels becoming a vaccinator is certainly feasible during elective surgery pauses. We recommend contacting your local vaccine team if you are interested in contributing to the coronavirus vaccination programme.
References
- Ferguson D, Cuthbert R, Karam E, Dott C, Wickramarachci L, Parker P, et al. UK Orthopaedic Trainees Covering Medical COVID-19 wards still meeting Joint Committee on Surgical Training trauma procedure guidelines: A successful multifaceted collaborative model. The Transient Journal, September 2020. Available at: www.boa.ac.uk/resources/knowledge-hub/uk-orthopaedic-trainees-covering-medical-covid-19-wards-and-still-meeting-joint-committee-on-surgical-training-trauma-procedure-guidelines-a-successful-multifaceted-collaborative-model.html. [last accessed 22/01/2021].
- Public Health England (2020). Training Recommendations for COVID-19 Vaccinators. Available at: www.gov.uk/government/publications/covid-19-vaccinator-training-recommendations/training-recommendations-for-covid-19-vaccinators. [last accessed 22/01/2021].
- Public Health England & UK Department of Health and Social Care (2020). COVID-19: the green book, chapter 14a. Available at: www.gov.uk/government/publications/covid-19-the-green-book-chapter-14a. [last accessed 22/01/2021].
- UK Department of Health and Social Care and the Medicines & Healthcare products Regulatory Agency ( 2020). Information for Healthcare Professionals on Pfizer/BioNTech COVID-19 Vaccine. Available at: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/940565/Information_for_Healthcare_Professionals_on_Pfizer_BioNTech_COVID-19_vaccine.pdf. [last accessed 22/01/2021].
- Kew J and Morales A. (2021) ‘Astra pledges 2 million vaccine doses a week for U.K. effort’. Bloomberg. 13 January. Available at: https://www.bloomberg.com/news/articles/2021-01-13/astra-pledges-2-million-vaccine-doses-a-week-for-u-k-effort. [last accessed 23/01/2021].
- UK Department of Health and Social Care and the Medicines & Healthcare products Regulatory Agency (2020). Information for Healthcare Professionals on COVID-19 Vaccine AstraZeneca. Available at: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/948334/Information_for_UK_healthcare_professionals_on_COVID-19_Vaccine_AstraZeneca.pdf. [last accessed 22/01/2021].
- NHS England and NHS Improvement (2020). Summary of the legal mechanisms for administering the COVID-19 vaccine(s). Available at: https://www.england.nhs.uk/coronavirus/wp-content/uploads/sites/52/2020/12/C0990-legal-mechanisms-summary-15-jan-21.pdf. [last accessed 22/01/2021].
